Nearly all (97%) births in the commonwealth occur in a Pennsylvania hospital. Hospitals are committed to and invested in continuous improvement and collaboration with other health care providers, policymakers, patients, families, and other stakeholders to ensure access to high-quality, equitable maternal health care.

Recent trends underscore the importance of these efforts. Maternal health complications are on the rise. Racial disparities in maternal health outcomes are widening. And—amid workforce shortages, financial distress, and a worsening medical liability climate—fewer hospitals are able to sustain maternal health services, leading to care deserts and gaps in services, particularly in rural communities.
Addressing these challenges requires strong collaboration with a focus, not only on improving safe and equitable hospital care, but also on strengthening care coordination, closing gaps in primary care and behavioral health services, tackling social drivers of health, strengthening connections with community partners, and ensuring the long-term sustainability of accessible maternal health care throughout the commonwealth.
Hospitals are focused both on improving the care they provide and being leaders in confronting the challenges outside their walls that contribute to maternal health complications and disparities.
Action Plan for Maternal Health
 During 2023, HAP’s Board of Directors identified maternal health as a priority area of focus for quality improvement efforts and public policy and authorized creation of a member Task Force on Maternal and Child Health. The task force, made up of clinical and administrative leaders from across the commonwealth, met throughout 2024 to develop recommendations for Pennsylvania hospitals and policymakers to:
During 2023, HAP’s Board of Directors identified maternal health as a priority area of focus for quality improvement efforts and public policy and authorized creation of a member Task Force on Maternal and Child Health. The task force, made up of clinical and administrative leaders from across the commonwealth, met throughout 2024 to develop recommendations for Pennsylvania hospitals and policymakers to:
- Advance high-quality, equitable maternal health care.
- Expand access to safe maternal care across the commonwealth.
- Strengthen and diversify the perinatal and neonatal workforce.
In addition, the task force identified key opportunities for HAP to support these efforts through advocacy and other initiatives.
See the task force’s action plan.
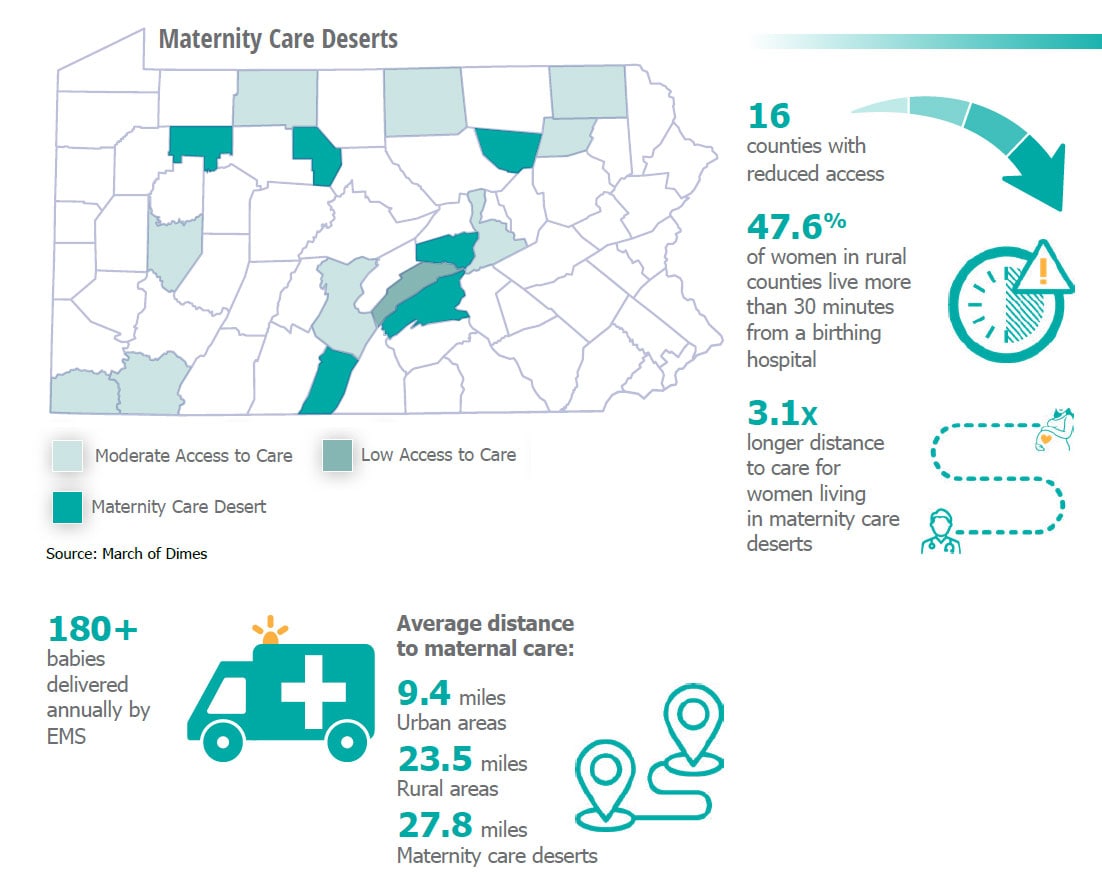
Maternity Care Deserts
Access to maternal health services is critical to improving outcomes. However, challenges such as maternal health deserts, hospital financial stability, and health care access disparities pose alarming risks to maternal health. As more obstetric units have been forced close across the commonwealth, maternity care deserts have increased.